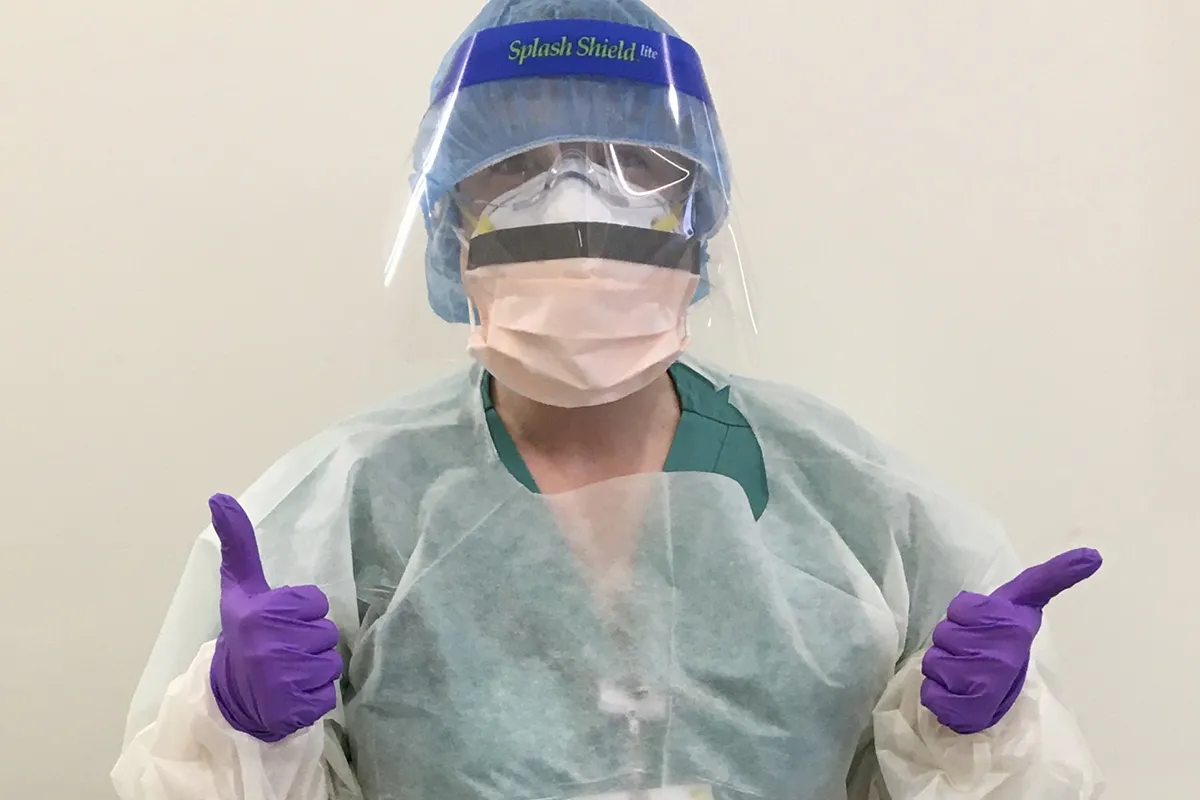
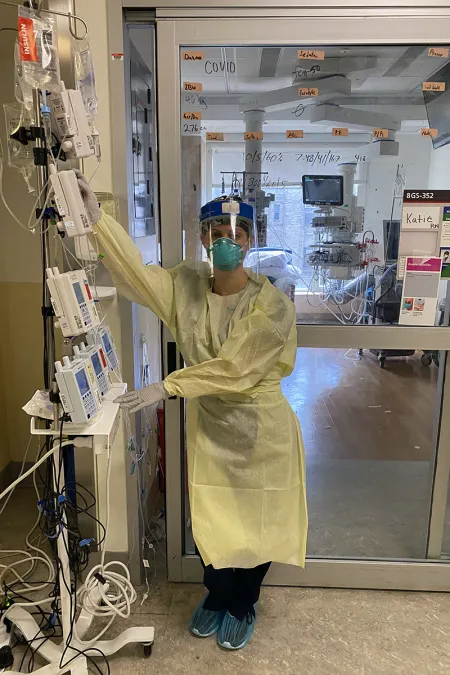
Katie Paccione ’12 still remembers the first time she donned the full PPE gear and walked into a COVID-19 room in New York-Presbyterian/Columbia University Medical Center. “There was a moment of holding my breath, not because I thought that if I breathed in I would get infected. I was like, ‘Okay, here we go.’’’
She understood the weight of the moment better than she’d understood the weight of all the gear: “It still feels heavy, and especially by the end of the shift, everything hurts because of that weight. But it felt especially heavy that first time.”
PPE is hot and sweaty, too. More than once, Paccione’s face shield slipped off completely, and she also nearly passed out from the heat — all potentially serious incidents that she lightly files under “oh, snap!” moments.
She said the question has never been whether she would get sick but when: “Every time you walk into that room, you have to wonder if this is it.”
Fear of catching the virus is a strong motivator said Susan Salahshor, a physician assistant who is the founding director of a new physician assistant program being launched soon at IC*, but the pressure to take physical precautions takes a mental toll.
“There has to be a healthy level of fear for you to say, ‘I need to be careful what I do,’” she said. But when does that healthy fear become something counterproductive, obsessive, or scarring? “That’s a very gray line, and that gray line is very thin. Almost every health care worker knows someone who has died, and of course they remember that episode. They know it only takes one mistake.”
Victoria Rainaud ’13, DPT ’15, a physical therapist working in New Jersey, always has her guard — and appropriate PPE — up, even with patients who aren’t yet known to be COVID-19 positive. “You’re going to be safest if you assume everyone has it. And that’s what we did, and so far, so good.”